- posted: Aug. 25, 2020
Keratoconus Treatment through Corneal Cross-Linking
What is Keratoconus?
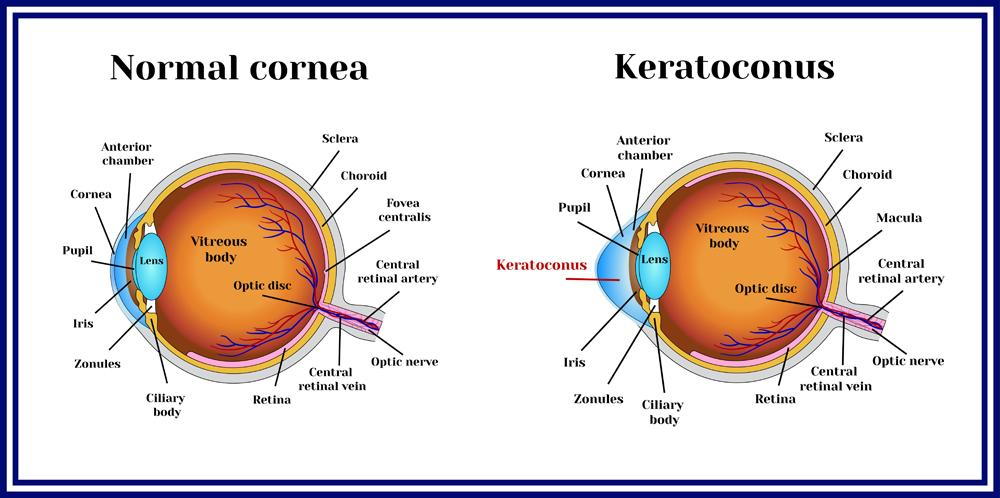
Keratoconus is a disorder in the eye where the cornea thins and gradually bulges outward into a cone shape.
Over time Keratoconus typically results in progressive thinning of your cornea, which can cause blurry vision (irregular astigmatism), double vision, myopia (nearsightedness), light sensitivity and/or glare.
While most people do not suffer from Keratoconus, this condition usually affects both eyes, although it often affects one eye more than the other eye. Severe cases of Keratoconus, patients may have scarring.
Source:- National Eye Institute (NEI) at the National Institute of Health: Corneal Disease discussion at NIE of NIH
For a more comprehensive discussion on Keratoconus please see the “WebMD Discussion: What is Keratoconus?”
What should you think you have Keratoconus?
Visit an eye doctor or ophthalmologist and have an eye examination.
How is keratoconus diagnosed?
During an eye exam, an eye doctor will use a slit lamp to diagnose you for Keratoconus. The curvature of your cornea will also be measured.
What Causes Keratoconus?
While the cause of Keratoconus is unknown, research indicates that the cause of Keratoconus is mostly due to a combination of genetic predispositions along with hormonal factors and environmental influences (such as allergies and rubbing your eyes).
Keratoconus is the most common corneal dystrophy in the U.S., affecting one in every 2,000 Americans (of which about 7% have a family history of this condition. Keratoconus is most prevalent in teenagers and adults in their 20s.
What Treatments Are Available for Keratoconus?
Keratoconus usually affects both eyes. In most cases, the cornea stabilizes after a few years without causing severe vision problems. Since Keratoconus is progressive, this condition will get worse over time,
Initially, Keratoconus can be corrected with glasses or soft contact lenses. If these treatments become less effective, then specially fitted contact lenses that correct the distortion of the cornea in order to improve vision may help.
As Keratoconus progresses it may cause irregular astigmatism that is not completely corrected by glasses or soft contact lenses. These eyes can usually be corrected to better vision with either hard gas permeable contact lenses or at times scleral lenses. For more information about hard gas permeable contact lenses, please see the WebMD discussion on “What Are Rigid Gas Permeable Lenses?“ For an update on Scleral Lenses, please see the AAO (American Academy of Ophthalmology) discussion “AAO- Update on Scleral Lenses” and the YouTube video Scleral Contact Lenses-Mayo Clinic.
A small number of people with keratoconus may develop severe corneal scarring or become unable to tolerate a contact lens. For these people, surgery may be the only viable option.
What Surgical Procedures Are Available for Keratoconus?
Corneal Cross-Linking and Corneal Transplants are two surgical options to treat Keratoconus when non-surgical treatments are not working. For most patients who need surgery to correct Keratoconus corneal cross linking is the best option.
In extreme and very severe cases, Corneal Transplants may be the only available surgical procedure. For more information on corneal transplants, please visit our “Corneal Transplants” discussion at Trusted LASIK Surgeons™.
Corneal Cross-Linking is a non-invasive procedure that is designed to stabilize and strengthen the cornea in order to slow or stop the progression of keratoconus. Keratoconus can be a hereditary condition or in very rare case can develop after LASIK surgery.
During the Corneal Cross-Linking procedure, a solution of riboflavin, which is a B vitamin, is applied to the cornea. The front surface of the eye is then exposed to a certain amount of UV light. This light activates a process where the riboflavin makes additional bonds between connective tissues and fibers in the cornea. The “cross-linkings” give extra rigidity and strength to the cornea.
What Happens during Cross-Linking Procedure?
A corneal eye surgery specialist is able to do this Corneal Cross-Linking procedure in his or her office.
First, you will have eye drops that numb your eyes. You can also get medicine that will help you stay calm if you and your doctor feel this is necessary.
Your eye surgeon then adds the formulated eye drops to your eyes. It will take about 30 minutes for the drops to make their way into the cornea. Then you lie back in a chair looking up at the light. Your eyes will be numb, so you should not feel any pain during this treatment. The entire
Corneal Cross-Linking procedure will typically take 60-90 minutes.
For an illustrative explanation about how the Cross-Linking procedure is performed, please see the YouTube video “Keratoconus Cross-Linking Procedure Explained” on the TV show “The Doctors.”
Types of Cross-Linking
There are two types of Corneal Cross-Linking surgery.
There is experimental epi-on and epi-off. The term “epi” is a shortened version for epithelium, which is the outer layer of the cornea. When your eye doctor uses the epi-off method, he or she will remove the epi before putting the drops in. With the epi-on method, the eye doctor just loosens the epi with a sponge or eye drops before putting the riboflavin drops in.
Should You Have Cross-Linking?
If you are suffering from Keratoconus, you may be wondering if you are a good fit for this treatment.
The procedure won’t reverse any changes keratoconus has caused, but it can keep these changes from getting any worse. Since corneal cross-linking can slow the progression of keratoconus, it’s better to start discussing any challenges you experience with your eyes with an eye doctor sooner rather than later because this is a progressive condition that gets worse over time, waiting can reduce the ability to minimize or treat this condition most effectively.
I Have Keratoconus—What’s Next?
Those with Keratoconus who are considering eye procedures (like LASIK or PRK surgery) may need to be treated with corneal cross-linking first. That is why we recommend finding a true expert in corneal and laser vision correction surgery since they can help recommend the best treatment for you and typically can perform the recommended surgical procedures.
Trusted LASIK Surgeons™ can help you find such experts in our Trusted LASIK Surgeons™ Directory. All LASIK surgeons featured in our directory are highly qualified LASIK experts and many of them Corneal Cross-Linking and some perform Corneal Transplants.
Even if a LASIK or Cataract surgeon you find in our directory near you does not perform Corneal Cross-Linking or Corneal Transplant surgery to correct Keratoconus, they can help you find the best surgeon to help you treat this condition.
Once you find a surgeon closest to you, please contact them directly by calling them or filling out their contact form from their website from the links we provide.
All LASIK and cataract surgeons featured at Trusted LASIK Surgeons™ are screened so you can be assured that each surgeon has proven expertise and one with professional accomplishments that have been recognized by their peers. To learn how we screen surgeons, please visit our discussion entitled
“How are surgeons screened at Trusted LASIK Surgeons™”?
Most of the LASIK surgeons at featured in our Trusted LASIK Surgeons™ Directory are also expert cataract surgeons and many perform other refractive procedures, like the Kamra Inlay, which can help with reading fine print (in books or on labels), lens implant procedures, and corneal transplants.
No matter what your vision problems are, Trusted LASIK Surgeons™ is here for you to help you find the best vision correction experts you can find.
Trusted Vision Surgeons, including vetted Trusted LASIK Surgeons® and Trusted Cataract Surgeons®
Trusted Vision SurgeonsTM is an online business that provides LASIK and Cataract Surgeon directories and consumer resources concerning eyesight and vision correction as well as a Consumer Checklist for the True Cost of LASIK.
Please Contact Us or call for more information.
Copyright ©2025 Trusted LASIK Surgeons® and Trusted Cataract Surgeons® All Rights Reserved.
Website Powered By iMatrix Ophthalmology

